
Dandelion Root Benefits: The Practitioner’s Guide to Liver, Gut, and Hormone Support

Dandelion root has a reputation problem. Most people know it as a weed, or maybe as a liver “detox” supplement with vague, unverifiable claims. Neither framing is particularly useful for practitioners.
The actual clinical picture is more interesting — and more specific. Dandelion root (Taraxacum officinale) has well-documented mechanisms for liver support, bile production, and gut microbiome health. Those three things are directly upstream of estrogen clearance, and that’s where it gets genuinely relevant for your hormone clients.
Here’s the breakdown.
Dandelion Root vs. Dandelion Leaf — Know the Difference
This distinction matters clinically and comes up constantly when clients start researching on their own.
- Dandelion root — higher concentrations of inulin (prebiotic fiber), taraxasterol (hepatoprotective), and the bitter compounds that stimulate bile. The right choice for liver support, microbiome work, and estrogen clearance.
- Dandelion leaf — stronger diuretic properties, higher mineral content (especially potassium). The right choice for clients with water retention or kidney support needs.
Most of the clinical research on hepatoprotection and gut health uses root preparations. When clients ask about “dandelion tea” they’ve seen online, it’s worth clarifying which part of the plant they’re actually getting.
| ROOT VS. LEAF — THE QUICK ANSWER FOR CLIENTS Root is for liver and gut. Leaf is for fluid and kidney support. They come from the same plant but they work differently.” |
What’s Actually in Dandelion Root

The bioactive compounds that drive the clinical effects:
- Taraxasterol — the primary hepatoprotective phytosterol. Modulates inflammatory and oxidative stress pathways in liver cells.
- Inulin — prebiotic fructan fiber. Concentration is highest in autumn-harvested roots. Selectively feeds bifidobacteria and lactobacillus.
- Taraxacin and taraxacerin — bitter sesquiterpene lactones. These are what stimulate bile production and digestive secretions.
- Polyphenols — chlorogenic acid, caffeic acid, luteolin, quercetin. Anti-inflammatory and antioxidant.
- Minerals — potassium (notable — one of the only bitter herbs that replenishes potassium alongside its diuretic effect), plus calcium, iron, manganese.
- Vitamins A, C, K — relevant for clients with nutrient depletion concerns on elimination diets.
What the Research Shows
1. Liver Support and Bile Production
This is dandelion root’s most documented mechanism and the one most directly relevant to your hormone clients.
The bitter compounds — taraxacin and taraxacerin — have both choleretic (stimulates bile production) and cholagogue (stimulates bile release) effects. A 2025 narrative review in MDPI Pharmaceuticals confirmed that taraxasterol modulates inflammatory and oxidative stress pathways in liver cells, with preclinical studies showing protection against liver damage from alcohol, carbon tetrachloride, and paracetamol.
Why does bile matter for hormones? Here’s the chain: the liver conjugates estrogen metabolites and packages them into bile for delivery to the intestines. If bile flow is sluggish, conjugated estrogens sit in the gut longer — giving beta-glucuronidase-producing bacteria more time to deconjugate and reactivate them. That means more estrogen gets recirculated instead of excreted.
Dandelion root addresses the upstream part of that problem. Better bile flow → more efficient estrogen delivery to the gut → better excretion.
| WHAT TO TELL CLIENTS Your liver packages used estrogen and sends it to your gut to be flushed out. Dandelion root helps keep that process moving — it’s supporting the exit pathway, not directly changing your hormone levels.” |
2. Gut Microbiome Support via Inulin
Dandelion root’s inulin content makes it a natural prebiotic. Inulin selectively feeds bifidobacteria and lactobacillus strains — the same bacterial groups most relevant to gut barrier integrity and immune regulation. Unlike chicory root inulin, dandelion root delivers this prebiotic activity alongside the bile-stimulating bitter compounds and taraxasterol, creating a liver-gut combination no isolated supplement replicates.
The microbiome connection to hormones runs through the estrobolome — the subset of gut bacteria that produce beta-glucuronidase and regulate estrogen reabsorption. A healthy, diverse microbiome supports estrobolome balance. Disrupted microbiome means dysregulated beta-glucuronidase activity, which means dysregulated estrogen recirculation.
To be clear: there is no human RCT directly linking dandelion root to estrobolome outcomes. The mechanism is logical — inulin feeds the bacteria, the bacteria regulate the estrobolome. Communicate it as the mechanistic inference it is, not as proven direct effect.
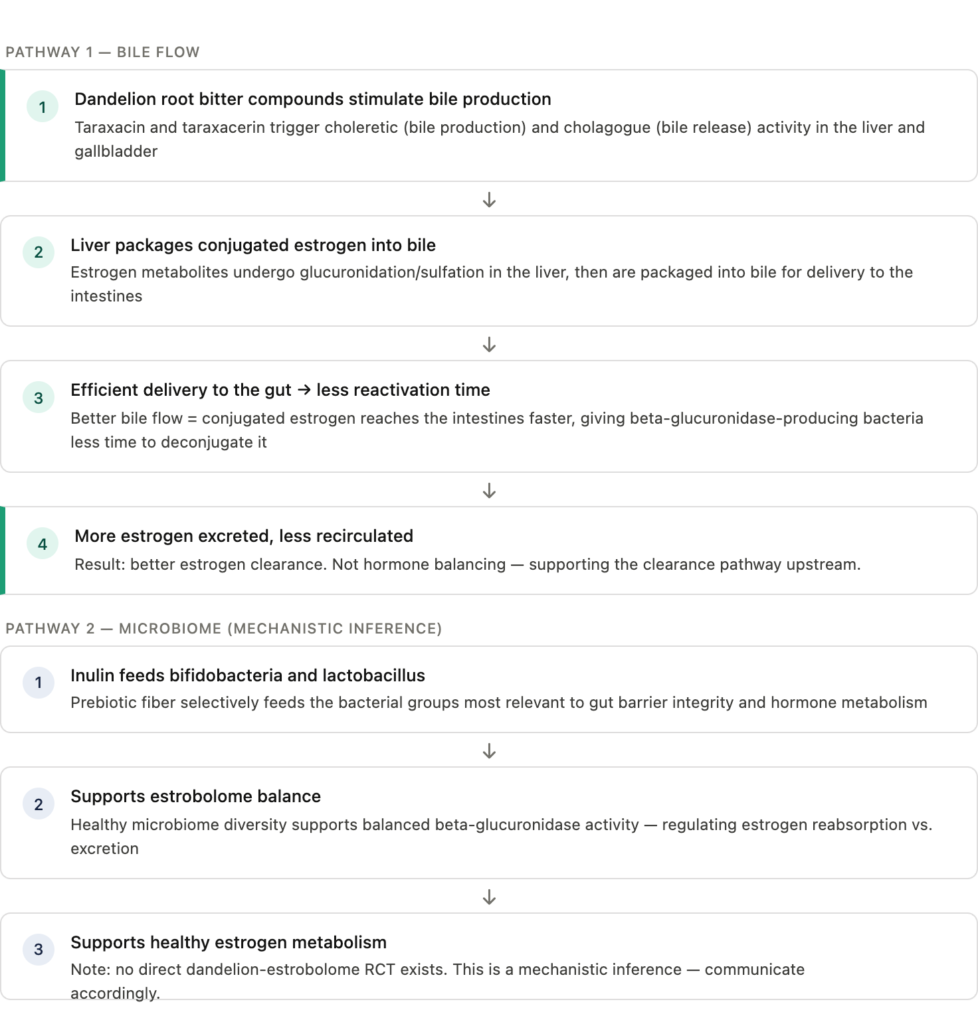
| THE MECHANISM CHAIN Dandelion root inulin → feeds bifidobacteria and lactobacillus → supports microbiome diversity → supports estrobolome balance → supports healthy estrogen clearance. Running in parallel: bitter compounds → stimulate bile → efficient estrogen delivery to gut → reduces reactivation time → supports excretion. |
3. Anti-Inflammatory Activity
Dandelion root’s polyphenol profile — luteolin, quercetin, chlorogenic acid, caffeic acid — provides anti-inflammatory activity through multiple pathways. Taraxasterol specifically modulates NF-κB-mediated signaling in preclinical models, reducing pro-inflammatory cytokine production.
There’s a completed clinical trial worth flagging here: NCT06625736 (October 6 University, Egypt / Pharos University Alexandria, 120 premenopausal obese women, completed September 2024) specifically measured dandelion extract’s effects on TNF-α, IL-6, IL-16, CRP, lipid profile, and glycemic indices over 3 months. Results had not been published at the time of writing — your fact-checker should verify this.
For AIP and Hashimoto’s clients: no thyroid antagonist compounds exist in dandelion root. No cross-reactivity with thyroid medications. The anti-inflammatory polyphenol profile is directly relevant to autoimmune load reduction.
4. Blood Sugar and Metabolic Support
Dandelion root’s inulin contributes to blood sugar regulation by slowing glucose absorption (soluble fiber effect) and supporting gut bacteria associated with improved insulin sensitivity. SCFA production from inulin fermentation — particularly butyrate — reduces intestinal inflammation and supports colonocyte health.
A completed RCT (NCT04054284, Croatia, 60 Type 2 diabetic patients, 12 weeks) evaluated a dandelion-containing herbal tea mixture’s effects on HbA1c and fasting glucose. Safety was the primary endpoint — the mixture was well-tolerated with no significant adverse events over 12 weeks. This is a safety signal more than an efficacy claim, but it’s relevant for practitioners recommending dandelion root to metabolic clients.

Protocol Compatibility — Quick Reference
| Protocol | AIP? | Wahls? | Anti-Inflam? | Notes |
| AIP Elimination Phase | ✓ Safe | ✓ Safe | ✓ Safe | No excluded compounds |
| Wahls Protocol | ✓ Beneficial | ✓ Beneficial | ✓ Beneficial | Polyphenol-dense, liver support |
| Anti-Inflammatory | ✓ Beneficial | ✓ Beneficial | ✓ Beneficial | Taraxasterol, luteolin, quercetin |
| Hashimoto’s | ✓ Beneficial | ✓ Beneficial | ✓ Beneficial | No thyroid antagonists |
| Perimenopause | ✓ Beneficial | ✓ Beneficial | ✓ Beneficial | Bile + estrobolome upstream support |
| Estrogen Dominance | ✓ Beneficial | ✓ Beneficial | ✓ Beneficial | Bile flow + microbiome diversity |
| SIBO (active treatment) | ✓ Can use | ✓ Can use | ✓ Can use | Inulin present — assess tolerance |
| Low FODMAP | ✓ Compliant | ✓ Compliant | ✓ Compliant | Well-tolerated at beverage dose |
| On levothyroxine | ✓ Safe | ✓ Safe | ✓ Safe | No absorption interference |
| On blood thinners | ⚠ Caution | ⚠ Caution | ⚠ Caution | Vitamin K content — assess dose |
| ONE CONTRAINDICATION TO KNOW Gallstones or bile duct obstruction are a contraindication. Dandelion root’s cholagogue effect — stimulating bile release — can trigger gallbladder attacks in clients with existing gallstones. Screen for this before recommending. Clients who’ve had their gallbladder removed are generally fine, but flag for individual assessment. |
Roasted Dandelion Root — Does Form Matter?
The roasting process concentrates bitter compounds and gives dandelion root a rich, earthy, coffee-like flavor that makes it practical as a daily beverage. Nutritionally, roasting doesn’t significantly reduce inulin or taraxasterol content.
There’s also a functional argument for the beverage format specifically. Consuming a bitter warm drink first thing in the morning activates the cephalic phase digestive response — the body’s anticipatory release of digestive secretions triggered by taste and smell. That primes bile flow and enzyme production before food arrives. A dandelion root beverage used as a morning ritual works differently than a capsule taken after breakfast.
For clients who’ve cut coffee and are looking for a morning ritual that supports liver and gut health, roasted dandelion root is a solid recommendation on its own. It also pairs well with roasted carob (SIBO-safe prebiotic fiber, D-pinitol for blood sugar) and chicory root (bifidobacteria-specific prebiotic). If your clients want all three in one drink, Sip Herbals makes a roasted blend using all three ingredients that’s AIP-compliant.
Common Questions
Is dandelion root AIP compliant?
Yes. Dandelion root contains no seeds, grains, nightshades, or dairy. It’s in the Asteraceae family (same as chicory, artichoke, milk thistle) and is AIP-compliant on the elimination phase. Clients with documented ragweed or daisy allergy should be flagged for Asteraceae cross-reactivity — but for most AIP clients it’s fully safe.
Is dandelion root safe for SIBO clients?
Generally yes, with nuance. Dandelion root contains inulin — the same fiber class as chicory root — but at beverage-level doses it doesn’t carry the same high FODMAP concern as concentrated chicory inulin supplements. For clients in active SIBO treatment, individual tolerance assessment still applies. Post-SIBO, dandelion root as a daily beverage is a clinically appropriate tool for rebuilding microbiome diversity.
Does dandelion root interact with levothyroxine?
No documented interaction. Coffee famously binds levothyroxine and reduces absorption — dandelion root doesn’t share that mechanism. For clients switching their morning ritual from coffee to a dandelion-based herbal beverage, levothyroxine absorption is likely to improve, not be affected. The standard 30–60 minute wait after medication before any food or beverage still applies.
Can dandelion root help with estrogen dominance?
The accurate answer: it supports the systems involved in estrogen clearance. Bile flow is upstream of estrogen excretion. Microbiome health is upstream of estrobolome function. Dandelion root addresses both. There’s no RCT directly measuring dandelion root and estrogen blood levels in humans — so frame it as supporting the clearance pathway, not balancing hormones directly.
Is there a difference between dandelion root tea and roasted dandelion root?
Standard dandelion root tea uses dried, unroasted chopped root steeped in water. Roasted dandelion root has a deeper, richer flavor from the roasting process, which also slightly concentrates bitter compounds. Inulin and taraxasterol content are similar in both. The choice between them is largely about palatability and ritual compliance.
Are there any side effects?
Dandelion root is well-tolerated at typical beverage doses. Occasional GI side effects (heartburn, loose stool) are reported at supplement doses, uncommon at beverage dose. Clients with gallstones should avoid it. Clients on warfarin should be assessed for vitamin K content. Asteraceae family cross-reactivity is possible in clients with ragweed allergy.
The Bottom Line
Dandelion root earns its place in a practitioner’s toolkit not because of one dramatic effect, but because of layered mechanisms that are directly relevant to common client concerns: sluggish bile flow, gut dysbiosis, estrogen clearance, and autoimmune inflammation.
The evidence is honest. Hepatoprotection is well-supported in preclinical models. Bile stimulation and prebiotic activity are well-characterized mechanistically. Direct human clinical trials on hormone outcomes are limited. The estrobolome connection is a logical inference, not a proven direct effect.
That’s a perfectly solid evidence base — as long as you communicate it proportionally. Clients who understand the mechanism are more likely to be consistent with it than clients who’ve been told it “balances hormones.”
WANT THE FULL PROTOCOL? Download The Anti-Inflammatory Morning Protocol — a free resource for practitioners working with gut and hormone clients. Includes a warm beverage comparison table, protocol-specific guidance, and client-ready language.
The Anti-Inflammatory Morning ProtocolSend download link to: |
References
1. Zarenezhad E et al. The Role of Dandelion (Taraxacum officinale) in Liver Health and Hepatoprotective Properties. Pharmaceuticals. 2025;18(7):990. MDPI
2. Osman AG et al. Hepatoprotection by dandelion (Taraxacum officinale) and mechanisms. Asian Pac J Trop Biomed. 2020;10(1). LWW Journals
3. Kania-Dobrowolska M, Baraniak J. Dandelion as a Source of Biologically Active Compounds Supporting Metabolic Syndrome Therapy. Foods. 2022;11(18):2841. PMC9497606
4. Anti-obesity Effects of Dandelion in Premenopausal Obese Women. NCT06625736. Completed Sept 2024. ClinicalTrials.gov
5. Safety and Efficacy of a Complex Herbal Tea Mixture in Type 2 Diabetics. NCT04054284. Completed Feb 2020. ClinicalTrials.gov
6. Clare BA et al. The diuretic effect in human subjects of an extract of Taraxacum officinale folium. J Altern Complement Med. 2009;15(8):929–34. PubMed 196787857. Baker LB et al. From Gut to Hormones: Unraveling the Role of Gut Microbiota in (Phyto)Estrogen Modulation. PubMed. 2024. PubMed 38342595
Written by Orleatha Smith, Master Herbalist & Co-founder, Sip Herbals | Fact-checked by | Last updated: April 2026

Orleatha Smith is a Master Herbalist and cofounder of Sip Herbals, with more than a decade serving the health and wellness community through science grounded, inclusive wellness education. She holds a Master’s Degree in Education, a biology teaching credential, and brings a rare mix of experience as a holistic lifestyle coach, SaaS developer, and organizational development specialist. Her work and insights have been featured in outlets including First for Women Magazine, The Los Angeles Times, and WebMD, alongside podcast and television appearances. Orleatha writes to help readers make practical, evidence informed wellness choices that fit real life.




